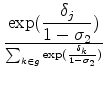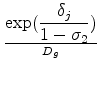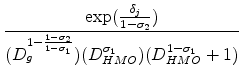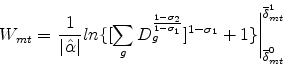Measuring the Return on Spending on the Medicare HMO Program
Keywords: Medicare, HMO, prescription drug benefits, welfare analysis, demand analysis
Abstract:
I estimate the welfare provided by and net costs of the Medicare HMO program in 1999-2002. I measure welfare with a nested logit model of demand for Medicare HMO plans using detailed data on plan benefits. From this, I derive estimates of consumer surplus and find that total welfare provided by the program over the four-year period is about $61 billion (2000 $). I also use data on favorable selection enjoyed by Medicare HMOs to estimate net costs, which total about $21 billion (2000 $). Net welfare therefore totals nearly $40 billion and the return on spending is about 186%.
"Medicare's payments for beneficiaries enrolled in Medicare Advantage plans are higher, on average, than what the program would spend if those beneficiaries were in the traditional fee-for-service (FFS) sector...Policymakers need to weigh that additional cost against the benefits provided by Medicare Advantage plans."
-Peter Orszag, director of the Congressional Budget Office in testimony to Congress, June 28, 2007
1 Introduction
The Medicare managed care program, in which commercial plans contract with the government to provide health insurance for Medicare beneficiaries, has existed in one form or another since 1972. In 1982, it took its modern form, where the government reimburses the plans a flat rate per month, and the plan bears the financial risk of providing insurance (Zarabozo 2000). Typically, the plans provide a more generous benefit package than that offered under traditional or fee-for-service (FFS) Medicare which probably partly explains why enrollees in Medicare private plans spend less than half out of pocket on health care than Medicare beneficiaries without any supplemental coverage at all (Neuman et al. 2007). Many of the plans charge enrollees a premium and, unlike FFS Medicare but like commercial managed care plans, restrict which doctors and hospitals enrollees can use and restrict what care an enrollee can receive.
The Medicare managed care program has caused controversy, however, because it raises the net cost of Medicare. The original goal of the program was to lower spending on Medicare by taking advantage of the managed care plans' supposed greater efficiency in providing insurance to beneficiaries. Because payments to the plans are only partly risk-adjusted, however, and because beneficiaries who choose managed care are in better health on average than those who stay in FFS Medicare, beneficiaries who enroll in a Medicare managed care plan end up costing more to the government than they would have if they had stayed in FFS Medicare. The program still seems to be valuable to beneficiaries, however, since, when many plans withdrew from the program earlier this decade following a reduction in their reimbursement, the outcry was considerable. The plans' reimbursements were restored in the Medicare Modernization Act of 2003 but were cut again for 2010 in April 2009.
In this paper, I offer some evidence on the welfare delivered by Medicare managed care plans, the costs of the Medicare managed care program, and on the return on spending on the program in the period 1999 through 2002. First, I estimate the consumer welfare offered by Medicare HMO plans in 1999 through 2002 using a nested logit model of demand for Medicare HMO benefits combined with data on HMO market shares and detailed benefit and premium data. I use the method presented in (Berry 1994) for estimating structural functions of demand for differentiated products with market share and product characteristic and price data and then calculate consumer surplus from the estimated demand function. My estimates show that Medicare beneficiaries in counties where managed care plans are present received $16.7 billion (in 2000 dollars) in consumer surplus in 1999; this amount rises to $16.9 billion in 2000 before dropping to $14.7 billion in 2001, and then to $12.5 billion in 2002.
To estimate the return on spending on the Medicare managed care program, I also calculate the net costs of the program. I do so by subtracting counterfactual spending (what the managed care enrollees would have cost Medicare in the FFS program) from actual spending on the managed care program as given in the financial reports of the Center for Medicare and Medicaid Services. To calculate what the managed care enrollees would have cost in the FFS program, I calculate what the average spending of a managed care enrollee in the FFS program would have been in each county by adjusting the average spending of a beneficiary in the FFS program in each county to reflect the managed care enrollees' lower expected spending. The adjustment is made by multiplying the average FFS spending by the ratio of the average risk factor of managed care enrollees to the average risk factor of FFS beneficiaries, as this ratio gives an estimate of what percent of FFS beneficiaries' spending managed care enrollees would be expected to have if they were in the FFS program. (The risk factor, which is calculated by CMS for each Medicare beneficiary based on his or her demographics and inpatient diagnoses from the previous year, gives the ratio of their expected spending to the average spending of an Medicare beneficiary.) I then multiply the average spending in each county by the number of managed care enrollees and aggregate over counties to get the total counterfactual costs for managed care enrollees in the FFS program.
Counterfactual spending on the Medicare HMO enrollees, when calculated in this way, is between $30 and $35 billion annually from 1999 through 2002. Actual spending on the Medicare HMO program was about $38 to $40 billion from 1999 to 2001, then dropped to $33 billion in 2002. Net costs of the program are around $6 billion per year from 1999 through 2001, and drop to $2.3 billion in 2002.
The return on government spending on the program is then calculated as the total welfare provided by the program divided by the net cost minus one. Total welfare is defined as counterfactual welfare (or welfare provided by FFS Medicare) subtracted from actual welfare provided by the Medicare HMO program. Since, in the demand model, however, the utility derived from being enrolled in FFS Medicare is normalized to zero, counterfactual welfare is also zero, so total welfare is simply equal to the welfare provided by the program. Over the four-year period, total welfare is about $61 billion (in 2000 dollars) and total net costs are about $21 billion; the program therefore provides net welfare of about $40 billion and the return on spending on the Medicare managed care program in this period is therefore about 186%.
The Medicare managed care program therefore not only provided positive net welfare and gave a positive return but the return was fairly high. Policymakers may wish to take this return into consideration when they decide to make changes to the program. The analysis presented here should be viewed in light of some caveats, however. First, it does not rule out that other policy options may deliver an even higher return. Second, in the years 1999 through 2002, the only plans available in the Medicare managed care program were health maintenance organizations (HMOs). Since the Medicare Modernization Act in 2003, however, the types of plans available in the Medicare Advantage program (as it was renamed) expanded to include preferred provider organizations (PPOs) and private fee-for-service plans. The private FFS plans may raise net costs more than the other types of plans as their payments tend to be higher (CBO 2007), which may lower the overall return on the program.
In measuring the welfare provided by the Medicare managed care program, I take an approach close to that of Town and Liu (2003) who estimate the welfare provided by the Medicare HMO program in 1993 through 2000 also using a nested logit model applied to market share data to estimate demand. This paper builds on that analysis in the following ways.
First, I take advantage of several datasets that were not available to Town and Liu (2003). One dataset I use has highly detailed data on the level of prescription drug benefits and on nondrug benefits. Town and Liu (2003) had no data on benefits available other than a dummy for whether or not the plans offered prescription drug benefits. I also use county-level data on per capita FFS spending and on the average risk factors of both FFS beneficiaries and Medicare HMO enrollees in order to estimate the net cost of the program. These data give direct information on the counterfactual costs of Medicare HMO enrollees for the exact counties and years under study.
Other changes in approach I make include using a more flexible nesting structure than Town and Liu (2003) did, that allows for correlation in utility across all managed care choices. I also instrument for premium with the premiums of competitors rather than the plan's own premiums, as using the plan's premiums may not be appropriate in the Medicare HMO context.
Taken together, these differences in approach give significantly different results for the welfare provided by and the net costs of the Medicare HMO program for the two years for which this paper and Town and Liu (2003) overlap (1999 and 2000). In their paper, consumer surplus for both years sums up to $8.3 billion, while spending on the program varies from net costs of $13.2 billion to a savings of $4.4 billion depending on their assumption about how much favorable selection Medicare HMOs experience. The results of their paper therefore range from the Medicare HMO program delivering a return of -37% to it delivering a simple benefit of $12.7 billion. I find, however, that consumer surplus in 1999 and 2000 sums up to $33.6 billion and net costs sum up to $12.6 billion, suggesting a return of 167% in those two years.
2 Background: the Medicare managed care program
Standard Medicare has high requirements for patient cost sharing relative to most modern private insurance plans. Medicare requires 20% co-insurance on most outpatient services, a high deductible ($812 in 2002) on hospital stays and only covers the first 150 days of hospitalization per year. To cover the remaining costs, a large proportion (88% in 2002) of beneficiaries have some kind of supplemental insurance. In 2002, 35% had employer-sponsored supplemental coverage, 21% had private Medigap insurance, 17% were on Medicaid and 15% were enrolled in a Medicare managed care plan (Kaiser Family Foundation 2005).
The Medicare managed care program was created to take advantage of the supposedly greater efficiency of private plans in providing health insurance for Medicare beneficiaries. (The program was called "Medicare+Choice" during 1999-2002, the period under study here, and is now called "Medicare Advantage.") Through the program, commercial plans contract with the Center for Medicare and Medicaid Services (CMS), the agency that runs Medicare, to provide health insurance for Medicare beneficiaries within a defined service area (for HMOs, a county or group of counties). The contract, which is revised and renewed each year, specifies benefits to be provided and possibly a premium that will be charged by the plan to the beneficiary, above the Medicare Part B premium which the beneficiary continues to pay. During the period studied here, the government reimbursed the plan at a flat rate that was set at a base level by county and then adjusted for the individual beneficiary's age, sex, Medicaid eligibility status, and employment status. The flat rate passed the financial risk of the beneficiary's medical care to the plan. Beneficiaries could enroll in the private plans or remain in FFS Medicare as they choose and were allowed to switch in and out of FFS Medicare or among plans whenever they want. The plans must either accept all Medicare beneficiaries as enrollees or close the plan completely.
The advantage of the managed care plans for the beneficiary is that they require less cost-sharing. Co-payments for doctor visits, for example, are usually about $10-$15 per visit, which is less than the 20% co-insurance required by FFS Medicare. Medicare managed care plans also often cover benefits that are not covered by FFS Medicare such as preventive care, vision care, dental care, and outpatient prescription drugs, which were not included as part of the standard Medicare benefit package before 2006. The primary disadvantage of Medicare managed care plans for beneficiaries, however, is that they usually require beneficiaries to see only providers within their network, while FFS Medicare places little constraint on what providers beneficiaries can see.
Neuman et al. (2007) find that Medicare beneficiaries enrolled in Medicare HMOs spend slightly less on average on health care than those in employer-sponsored retiree plans, about three-quarters of what is spent by those in Medigap plans, and less than half of what is spent by those without any supplemental coverage at all. These figures do not take into account differences in health status among the beneficiaries in the different options but still suggest that Medicare HMOs can offer considerable saving for some beneficiaries. They also find that beneficiaries in Medicare HMOs also have slightly lower incomes than those in employer-sponsored or Medigap plans suggesting that their choice of the HMO may reflect a lower demand for health insurance.
There is evidence that strongly suggests that beneficiaries who choose to enroll in Medicare managed care plans are in better health and therefore have expected lower health-care spending on average than the beneficiaries who stay in FFS Medicare. Several studies, using Medicare claims data, have found that beneficiaries who enroll in Medicare HMOs had lower health-care spending before enrolling than beneficiaries who chose to remain in FFS Medicare (Cox and Hogan 1997, GAO 1986, Morgan et al. 1997, Thiede et al. 1999). Estimates of the spending of beneficiaries who later join HMOs as a percent of the spending of beneficiaries who remain in FFS Medicare ranged from 63 percent to 71 percent. Other studies, using the Medicare Current Beneficiary Survey or other surveys, find that HMO enrollees have better self-reported health status and fewer impairments (Brown et al. 1993, Banthin and Taylor 2001, Atherly et al. 2004, Mello et al. 2003).
The most comprehensive and up-to-date evidence on this question is provided by Greenwald et al. (2000). In early 2000, CMS implemented a method for risk adjusting payments to Medicare HMOs by modelling each beneficiary's expected health care spending as a function of their demographics and inpatient diagnoses in the previous year. The resulting risk factor is calculated as the ratio of the individual's beneficiary expected health care spending to the average expected health care spending of a beneficiary enrolled in the FFS program. Greenwald et al. (2000) compare the average risk factors of FFS Medicare beneficiaries with Medicare HMO enrollees for all counties with Medicare HMOs calculated based on inpatient data from 1997-98. They find that, in the median county, the average risk factor of HMO enrollees is nearly 14 percent below the average risk factor of beneficiaries in FFS Medicare and that the vast majority of counties have favorable selection in the managed care population to some degree.
From 1982 through 1997, managed care plans who contracted with Medicare were reimbursed 95 percent of the expected spending of beneficiaries in FFS Medicare. The research from the early 1990s cited above, however, raised concerns that the plans were being overpaid, as it became clear that managed care enrollees cost on average less than 95 percent of what beneficiaries who stayed in the FFS program. In 1997, the Balanced Budget Act lowered the growth rate of reimbursements to the plans in many counties. As a result, however, many plans withdrew from the program; the number of contracts dropped from 407 in 1999 to 240 in 2002, and many beneficiaries were involuntarily disenrolled from their plan, which led to outcry by the enrollees because of the loss of the benefits from the plans.1
In response, the Medicare Modernization Act of 2003 greatly increased reimbursement for private plans in the program. Whereas before the Balanced Budget Act, private plans were paid 95% of what an average beneficiary was expected to cost in FFS Medicare, in 2005, private plans were paid about 112% of average costs in FFS Medicare (Biles et al. 2006). The reaction among plans was strong; the number of contracts rose to 602 by 2007, and enrollment in private plans expanded from 5.3 million beneficiaries in 2003 to 8.7 million beneficiaries in 2007. The program is still often criticized on the grounds that it raises costs for Medicare, however, and in April 2009, the plans' reimbursement was cut again.2
3 A model of demand for Medicare HMO benefits
To estimate the welfare provided by the extra benefits of Medicare HMO plans and by the lower out-of-pocket spending of Medicare HMO enrollees, I first estimate a structural model of demand for Medicare HMO benefits. Berry (1994) showed that, by inverting the function relating market shares to utility, it is possible to estimate ordinary and nested logit models of demand using linear regressions on aggregate data. The example he used was a two-level model where the choices are grouped exhaustively into G groups, other than one choice which is referred to as the "outside" choice and for which consumer surplus is normalized to zero.
Town and Liu (2003) apply this model to the demand for Medicare HMOs. They sort the HMOs into two nests by whether or not they offer prescription drug benefits while defining remaining in FFS Medicare as the outside choice. A potential problem with their approach, however, is that, intuitively, we would expect all the managed care choices to be nested together since managed care plans have many features in common, such as limited provider choice, demand for which is probably correlated across plans for the same individual.
I therefore nest all the managed care choices together. In addition, like Town and Liu, I nest them within that nest by whether or not they offer prescription drug benefits. Utility of individual ![]() for plan
for plan ![]() in this model is given by:
in this model is given by:
| (1) | |||
![]() consists of the observed characteristics of the choices, and
consists of the observed characteristics of the choices, and ![]() is a scalar
measuring the quality of the choice observable to the consumer, but not to the econometrician. These together make up
is a scalar
measuring the quality of the choice observable to the consumer, but not to the econometrician. These together make up ![]() , which is the part of utility that is the same for choice
, which is the part of utility that is the same for choice
![]() across individuals. Each individual also has a random draw of utility
across individuals. Each individual also has a random draw of utility ![]() for the managed-care nest, a random draw of utility
for the managed-care nest, a random draw of utility ![]() for each prescription-drug nest
for each prescription-drug nest ![]() , and a draw
, and a draw ![]() for each plan. Each individual chooses the plan
for each plan. Each individual chooses the plan ![]() that gives them the maximum utility.
that gives them the maximum utility.
The parameters ![]() and
and ![]() (both
(both ![]() ) measure the correlation in unobserved utility across choices in the same nest. As the parameters approach one, within-nest substitution is stronger than across-nest substitution.
) measure the correlation in unobserved utility across choices in the same nest. As the parameters approach one, within-nest substitution is stronger than across-nest substitution. ![]() measures the correlation in unobserved utility across all the managed-care choices and
measures the correlation in unobserved utility across all the managed-care choices and ![]() measures the
correlation in unobserved utility across the plans within the two prescription-drug nests.
measures the
correlation in unobserved utility across the plans within the two prescription-drug nests.
The estimating equation for this model is derived as follows. (The derivation is similar to Berry's for the two-level model.) The share of plan ![]() within prescription-drug nest
within prescription-drug nest ![]() is given by:
is given by:
The share of nest ![]() within the HMO group is in turn given by:
within the HMO group is in turn given by:
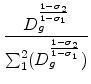 |
(3) | ||
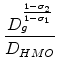 |
Finally, if we normalize
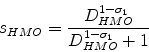 |
(4) |
| (5) |
The unconditional share of plan ![]() is therefore:
is therefore:
Algebraic manipulation similar to Berry (1994)'s for the two-level model yields the following equation that can be used to estimate ![]() ,
, ![]() , and
, and ![]() :
:
| (7) |
The difference between this equation and Berry (1994)'s equation for the two-level model is that Berry (1994)'s equation omits
![]() as a regressor, forcing
as a regressor, forcing ![]() to be 0. If
to be 0. If ![]() is correlated with
is correlated with ![]() , however, omitting it leads to inconsistent estimation of
, however, omitting it leads to inconsistent estimation of
![]() and
and ![]() . To test which is the preferred model, I will include
. To test which is the preferred model, I will include
![]() ; if the coefficient
; if the coefficient ![]() is significantly different from
zero, the estimates from the two-level model will be biased, and the three-level model would be more appropriate.
is significantly different from
zero, the estimates from the two-level model will be biased, and the three-level model would be more appropriate.
4 Data on Medicare HMOs in 1999-2002
Data were collected for the years 1999 through 2002. Market shares for Medicare HMOs come from the Medicare Managed Care Market Penetration State/County/Plan Data files, which contain enrollment in Medicare managed care plans by plan, county, and month; I use the files for June of each year. Reimbursement levels come from the Medicare+Choice Payment Rate files and the base reimbursement rate for the aged in each county is used. Benefit and premium data come from the Medicare Compare database, which is the database underlying the online plan chooser for Medicare beneficiaries. All of these data sources were obtained from the Center for Medicare and Medicaid Services (CMS), the government agency that runs Medicare.
The enrollment data give enrollment by contract number within a county. One contract may, however, cover more than one package of benefits since HMOs are allowed to offer more than one within a county. Usually, the offerings consist of a "basic" plan with an optional supplement for an extra premium. Since enrollment is not split up by packages however, I attribute all of the enrollment to the HMO's "basic" plan, defined as the plan with the lowest premium. (Atherly et al. 2004 report that 87% of Medicare HMO enrollees with prescription drug coverage receive it through the plan's basic benefit package.)
The market share for each plan was calculated by dividing the plan's enrollment by the number of Medicare eligibles in the country, adjusted to reflect state-level rates of Medicaid and employer-sponsored plan participation because beneficiaries who were eligible for those programs are likely to choose them over a Medicare HMO. These rates were calculated by pooling the March demographic supplements of the Current Population Survey for the four years, identifying respondents reporting being covered by Medicare and then tabulating the rates at which these respondents also report being covered by Medicaid and employer-sponsored insurance by state. It was necessary to use state-level rates and to pool the years since the sample sizes for MSAs or for individual years would not have been large enough.
During the years 1999-2002, the Medicare managed care program contracted, as numerous plans left the program in response to provisions in the Balanced Budget Act of 1997 which lowered the growth rate in their reimbursements. Table 1 shows the decline in the number of plans participating in the program and in the number of counties with at least one Medicare HMO available. The number of plans participating declined from 280 in 1999 to 139 in 2002 and the number of counties with plans declined from 794 to 540 over the same period.
As Table 1 also shows, Medicare HMOs have a small but substantial presence in the counties of their service areas. The average Medicare HMO market share is about 11%, and the average enrollment in a Medicare HMO is about 3,900. The market share of FFS Medicare is, on average, about 75%.
In addition to many HMOs dropping out of the program during this period, a further effect of reducing the reimbursement was that the HMOs who stayed in raised premiums faster than the rate of inflation and reduced coverage. Table 2 shows the average premiums (in 2000 dollars) charged by Medicare HMOs and average benefits provided by them by year. The average premium more than tripled from $12 to $37 between 1999 and 2002 while at the same time the percentage of plans offering prescription drug benefits dropped from 73% in 1999 to about 52% in 2002.
If Medicare HMO plans offered prescription drug coverage, they could offer only coverage of generic prescription drugs or also offer coverage for brand-name prescription drugs. Table 2 also shows that the percent of plans offering brand-name prescription drug coverage drops from 69% in 1999 to 35% in 2002. The percent of plans offering only coverage of generic drugs therefore rises from almost 4% in 1999 to about 17% in 2002.
If Medicare HMOs offered brand-name prescription drug coverage, they nearly always put a limit on that coverage. Table 2 also shows that the mean annual coverage limit (in 2000 dollars), given that plans offered brand-name prescription drug coverage, dropped from about $703 in 1999, to about $253 in 2002.
The Medicare Compare database also contains extensive information on the nondrug benefits of the plans. For the purposes of this paper, information about the following benefits were extracted: the co-payment for a primary care visit, the co-payment for a specialist visit, the inpatient deductible, whether or not the plan required a referral to see a specialist, whether or not it offered vision benefits and whether or not it offered dental benefits.
As Table 2 shows, both of the average doctor visit co-payments increased slightly between 1999 and 2002: the primary care co-payment from about $8 to about $10, and the specialist co-payment from about $9 to $15. The average deductible for inpatient hospital stays more than sextupled during the same period, from $21 to $132. The percentage of plans that do not require a referral to see a specialist is very small but rises noticeably in 2002.
The plans also have the option of offering vision and dental benefits above the level of FFS Medicare. FFS Medicare's vision benefits only cover exams for glaucoma for high-risk patients, and glasses following cataract surgery. The HMOs typically cover routine eye exams and/or glasses and contact lenses. FFS Medicare has almost no dental coverage, while the HMOs, if they offer dental coverage, cover from one to an unlimited number of preventive dental exams. Since information about vision and dental coverage was sometimes incomplete, however, I only control for whether they offer each kind of coverage, not what the level of coverage is. As Table 2 shows, most plans offer vision benefits and the percentage of plans offering vision benefits declines only slightly, from 93% in 1999 to 85% in 2002. The percentage of plans offering dental benefits more than halves, from 32% in 1999 to 14% in 2002.
5 Empirical strategy
As discussed in Section 3, the regression to be estimated is:
| (8) |
![]() contains characteristics of the plan that are unobserved by the econometrician but are observed by the beneficiaries and affect their valuation of the plan. Among other things, it
might include the extensiveness and quality of the HMO's provider network.
contains characteristics of the plan that are unobserved by the econometrician but are observed by the beneficiaries and affect their valuation of the plan. Among other things, it
might include the extensiveness and quality of the HMO's provider network.
These unobserved characteristics are correlated with premium, the log of the plan's share within its nest (
![]() ), and the log of the nest's share within the total HMO share of the market (
), and the log of the nest's share within the total HMO share of the market (
![]() ). In order to partially overcome this problem, I use plan-county fixed effects which capture the plan-county mean quality
). In order to partially overcome this problem, I use plan-county fixed effects which capture the plan-county mean quality
![]() and leave the time-specific deviation in plan quality
and leave the time-specific deviation in plan quality
![]() as the error term. This strategy for dealing with the correlation between price and unobserved quality is very similar to that of Hausman (1997) and Nevo (2001). The only
potential remaining inconsistency in estimation therefore would arise from factors that change over time for a given plan in a given county that affect both their premium and conditional shares, and demand for their product.
as the error term. This strategy for dealing with the correlation between price and unobserved quality is very similar to that of Hausman (1997) and Nevo (2001). The only
potential remaining inconsistency in estimation therefore would arise from factors that change over time for a given plan in a given county that affect both their premium and conditional shares, and demand for their product.
To deal with this remaining concern, the premium, the log of the plan's share within its nest (
![]() ), and the log of the nest's share within the HMO group (
), and the log of the nest's share within the HMO group (
![]() ) are all instrumented. Two instruments for the premium are used. The first is created by calculating the mean of the premiums charged by the plan's competitors for each
of the other counties in the plan's service area, and then calculating the mean of these means, weighted by the number of Medicare eligibles in each county. The weighting takes into account the relative importance of the other markets to the plans' pricing decisions.
) are all instrumented. Two instruments for the premium are used. The first is created by calculating the mean of the premiums charged by the plan's competitors for each
of the other counties in the plan's service area, and then calculating the mean of these means, weighted by the number of Medicare eligibles in each county. The weighting takes into account the relative importance of the other markets to the plans' pricing decisions.
For example, in 2002, Harvard Pilgrim Health Care offered a Medicare HMO plan in Essex, Middlesex, Suffolk and Norfolk counties in Massachusetts. Tufts HMO and Blue Cross/Blue Shield also offered Medicare HMO plans in Middlesex, Suffolk, and Norfolk counties, and Fallon Health Plan offered one in Norfolk County. The instrument for the Harvard Pilgrim Health Care-Essex County-2002 observation would be calculated by taking the means of Tufts and Blue Cross Blue Shield's premiums in Middlesex County, of the same two plans' premiums in Suffolk County and of the premiums of Tufts, Blue Cross Blue Shield and Fallon in Norfolk County, and then calculating the mean of these three numbers weighted by the number of Medicare eligibles in each of the three counties.
This variable is a valid instrument because of the particular regulatory requirements placed on Medicare HMOs. Medicare HMOs set premiums only once a year, in their contract with CMS, and with a large lead time, as proposals are due in late spring for contracts to take effect the following
January. If we assume that, at the time they are contracting with CMS and setting their premiums, the competitors are unaware of changes in the network of the plan and county of the observation (in other words, of changes in the error term,
![]() ), competitors' premiums are independent of the error term. Competitors' premiums in other counties are, however, correlated with the premium of the observation through the
components of marginal cost common across the region.
), competitors' premiums are independent of the error term. Competitors' premiums in other counties are, however, correlated with the premium of the observation through the
components of marginal cost common across the region.
In using competitors' premiums, this paper differs from most previous work in this area, which use the firm's own prices in other geographic regions as instruments rather than competitors' prices (Hausman 1997, Nevo 2001). The assumption behind using the firm's own prices is that shocks to marginal cost will be reflected in the firms' prices across counties. That strategy requires, however, the assumption that the different regions' deviations from the mean valuation of the same good be independent of each other. This assumption can be justified in the case where regions are geographically separated from each other and the good that is being sold is identical across regions (as in the case of ready-to-eat cereal being sold in different cities across the US, as in Hausman [1997] and Nevo [2001]). Medicare HMOs, however, tend to operate in a group of counties that are contiguous and beneficiaries are likely to be crossing over county boundaries to receive their medical care. In this case, the time-specific deviations from the means of quality in each county are not going to be independent of each other in adjacent counties for the same plan, limiting the applicability of the type of instrument used in previous work. I therefore use competitors' premiums, as described above.
The other instrument for premium is the base reimbursement rate for the county since that is an exogenous determinant of price. The reimbursement rate is set by legislation and is the same for all plans within a county.
To instrument for the logs of the conditional shares, I use functions of the characteristics of other firms in the same market. These variables will capture the part of the firm's share of its nest that is determined by other firms' behavior but not the part that is set by the firm's own characteristics. The instruments for the plan's share within its drug/non-drug nest are therefore the means of the brand-name drug coverage amount and the means of the non-drug benefits offered by competing plans in the same drug/non-drug nest in the same county. If there are no other plans in the same drug/non-drug nest, these are set to zero. The instruments for the drug/non-drug nest's share of the overall HMO share are the means of the same variables for the plans in the other drug/non-drug nest within the same county. If there are no plans in the other nest, these are also set to zero.
In the demand regressions, drug benefits are specified both with a simple dummy for the plan offering drug benefits and with a more detailed specification of drug benefits. The first specification allows direct comparison with other studies with less detailed drug benefit data, such as Town and Liu (2003). The second specification includes a dummy for generic prescription drug coverage, the brand-name prescription drug coverage amount, and the brand-name prescription drug coverage amount squared. The coverage amounts are deflated to 2000 levels using the Consumer Price Index for prescription drugs.
Finally, dummy variables for years are included to control for yearly shifts in demand for HMOs and their associated medical care.
6 Demand results
Table 3 reports the results of estimating the demand equation for the two different specifications of drug benefits and for ordinary logit, Town and Liu (2003)'s two-level nested logit model, and the three-level nested logit model. Which specification used does not significantly affect the coefficients on premium. The coefficient on premium is -0.005 in the ordinary logit with the detailed drug benefit specification and -0.007 in the two nested models, with a standard error of 0.001 in all models.
When we compare the results for the three utility specifications (logit, two-level nested logit, and three-level nested logit), we see that, since ![]() is estimated to be .5 in the
three-level nested logit model (when drug benefits are specified in detail) with a standard error of .1, this latter model is the preferred one. This model allows beneficiaries' utility functions to be correlated across all managed-care choices. The positive and significant estimate for
is estimated to be .5 in the
three-level nested logit model (when drug benefits are specified in detail) with a standard error of .1, this latter model is the preferred one. This model allows beneficiaries' utility functions to be correlated across all managed-care choices. The positive and significant estimate for
![]() means that failing to allow for this correlation will lead to the estimates of the effects of the benefits being inconsistent, and that we should therefore focus on the results from
the three-level nested logit.
means that failing to allow for this correlation will lead to the estimates of the effects of the benefits being inconsistent, and that we should therefore focus on the results from
the three-level nested logit.
The estimated effects of the benefits mostly have the expected sign, with the exception of the dummy for generic coverage which is weakly negative. The remaining benefits mostly have estimated effects that are significant; the exceptions are the two doctor visit co-payment variables, and the dummy for dental benefits.
To make the magnitudes of the effects shown in Table 3 clearer, Table 4 translates the marginal utilities given in Table 3 into willingnesses to pay by dividing the marginal utilities of the benefits by the marginal utility of income as estimated by the coefficient on premium. Table 4 gives the results of this calculation for the three models (ordinary logit, two-level nested logit, and three-level nested logit), both specifications of drug benefits, and for the nondrug benefits in the equations where drug benefits are specified in detail. Since the premium was deflated to 2000 dollars in the demand regressions, the estimates of the willingnesses-to-pay are therefore also in 2000 dollars.
While the differences across the equations are generally not significant, the point estimates of the effect of drug benefits drop noticeably in the three-level model. The marginal willingness to pay for a drug benefit is estimated to be about $14 in the two-level model but $8 in the three-level model (and the estimate is insignificantly different from zero in the latter). Similarly, the willingness to pay for the first $100 of monthly brand-name coverage drops from $23 in the two-level model to $18 in the three-level model.
For the nondrug benefits, the estimates of the three-level model show that beneficiaries are willing to pay about $1 per month to reduce the primary care co-payment by $1, $0.54 per month to reduce the specialist co-payment by $1, about $2 per month to reduce the inpatient deductible by $100, about $38 per month to remove the requirement to seek a referral before seeing a specialist, about $8 per month for dental benefits, and about $15 per month for vision benefits. All but the last estimate are significantly different from zero.
There is little information or other estimates to which these estimates can be compared, or against which they can be benchmarked. The response to the primary care co-payment can be characterized as strong, since a willingness to pay $1 per month to reduce the primary care co-payment by $1 implies that, if beneficiaries are rational, they are visiting their primary care doctors once a month on average. According to the Medicare Current Beneficiary Survey, however, the median number of visits to the doctor made by Medicare beneficiaries is six per year, or one every other month (Kaiser Family Foundation 2005). It is hard to know why enrollees are reacting so strongly to the primary care co-payment; it is possible that they are overreacting to it simply because it is usually listed first in the output of the Medicare Compare database. For the other benefits, there is little to benchmark the estimates of their effects against.
7 Beneficiary welfare provided by the Medicare HMO program
The next section uses the demand function estimated in the previous section to calculate the consumer welfare provided by the Medicare HMO program from 1999 to 2002. As Small and Rosen (1981) show, surplus per consumer in a market in a discrete-choice model is found by integrating over the share function. Intuitively, this result is analogous to the result for continuous choice that compensating variation is found by integrating over the compensated demand function. For a representative consumer, the compensating variation of a change either in the number of choices available, or their characteristics is given by:
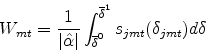 |
(9) |
![]() is the vector of mean utilities from the choices available before the change and
is the vector of mean utilities from the choices available before the change and
![]() is the same vector after the change. As Small and Rosen (1981) show, this integral can be applied to multiple changes in choice characteristics or in the number of choices
at once.
is the same vector after the change. As Small and Rosen (1981) show, this integral can be applied to multiple changes in choice characteristics or in the number of choices
at once.
If we integrate the share formula for the three-level nested logit model (equation 6) in this way, we obtain:
where, as in equation (2),
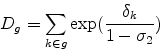 |
(11) |
Table 5 shows beneficiary welfare provided by the Medicare HMO program calculated from this formula. In the first row, monthly compensating variation per Medicare eligible was calculated as in equation (10) for each county and averaged across counties, weighting by the number of eligibles in each county. As it shows, average monthly compensating variation per beneficiary was $85 in 1999, rose to $86 in 2000, and then dropped to $80 in 2001, and further to $71 in 2002. The differences across the years are not statistically significant, however. The changes in average welfare are due both to changes in the plans' benefits and changes in the number of choices due to plans entering and withdrawing the program.
The third row of table 5 shows aggregate annual welfare from the Medicare HMO program. Aggregate annual welfare is calculated by multiplying average monthly compensating variation in each county by the number of Medicare eligibles in the county, summing up total compensating variation over the counties, and multiplying by twelve:
| (12) |
Estimated aggregate welfare is given in the last row of Table 5. As the table shows, aggregate welfare is estimated to be $16.7 billion in 1999. This estimate rises to $16.9 billion in 2000, and then falls to $14.7 billion in 2001 and further to $12.5 billion in 2002. The decline from 2000 to 2002 is due both to the drop in average consumer surplus per beneficiary (because plans raised their premiums and cut their benefits), shown in the first row of Table 5, and to the drop in the number of beneficiaries who have a plan available to them, shown in the second row of the table.
8 Net cost of the Medicare HMO program
The net cost of the Medicare HMO program to the government is the actual amount spent on the program by the government minus the amount the government would have spent on medical care for the Medicare HMO enrollees if they had been enrolled in FFS Medicare.
Table 6 presents calculations of the actual amounts spent on the Medicare HMO program in calendar years 1999-2002. These calculations are based on the financial reports for the Centers for Medicare and Medicaid Services (CMS) for fiscal years 2000-2003. The first line of the table shows the amounts given for the "Program/Activity Costs" for Medicare managed care in "Note 10: Net Cost of Operations" in each report in nominal billions of dollars. In fiscal year 2000, Medicare spent $39.8 billion on the managed care program; this figure rises to $42.0 billion in fiscal year 2001, then drops to $33.8 billion in fiscal year 2002 and rises again to $36.4 billion in fiscal year 2003.
Since fiscal years in the federal government begin on October 1 of the calendar year preceding the year with the same number as the fiscal year, spending for calendar years 2000-2002 (shown in the second line of the table) was calculated by taking a weighted average of the spending in the two fiscal years covered, with a three-quarters weight on the spending for the fiscal year with the same number and a one-quarter weight on the spending for the fiscal year with the preceding number. The second line also shows the amounts deflated to 2000 levels by the GDP deflator. Spending in calendar year 2000 is estimated to be $38.2 billion; this figure drops to $36.2 billion in 2001, and drops further to $32.3 billion in 2002.
The financial report for CMS for fiscal year 1999 was not available, however, so spending on the Medicare managed care program for the first nine months of 1999 was estimated in the following way. Spending on the Medicare managed care program in each year is assumed to have two components: reimbursements to plans and administrative expenses. Data on reimbursement rates and enrollment for the years 1999 through 2002 are directly available from CMS; reimbursements to plans in each county and year are given by the base reimbursement rate for each Medicare eligibility category (aged, disabled, and end-stage renal disease) in that county and year multiplied by the enrollment for each category in that county and year and added up across categories. Then this spending is added up across counties for each year to give total reimbursements for the Medicare managed care program. The third line of Table 6 shows the results of this calculation: total reimbursements to plans were $36.5 billion in 1999, $38.2 billion in 2000, $36.2 billion in 2001, and $32.3 billion in 2002. (The reimbursement rate has been inflated to 2000 levels with the GDP deflator.) For the years 2000-2002, for which both the amount spent on the program according to the financial reports and the total reimbursements to plans are available, the amount spent on administration is calculated by subtracting the former from the latter. This amount is reported as a percentage of reimbursements in the fourth line of Table 6 and is calculated to be 5.6% in 2000, 7.9% in 2001, and 2.4% in 2002. For 1999, administrative expenses as a percent of reimbursements are assumed to be 5.3%, the average of the percentages in 2000-2002. Total spending on the program in 1999 is therefore $38.4 billion, or 5.3% above the total reimbursement amount of $36.5 billion. Total actual spending on the Medicare managed care program in 2000 dollars (the last line of Table 6) is therefore $38.4 billion in 1999, $40.4 billion in 2000, $39.0 billion in 2001, and $33.1 billion in 2002.
Next I show the calculation of how much the Medicare program would have spent if managed care enrollees in 1999 through 2002 had been enrolled in FFS Medicare instead. Briefly, my method is to take the average amount spent per beneficiary in the FFS program (reported by CMS for each county), adjust it for favorable selection with regard to health status in the Medicare managed care program, and sum it up over counties for each year; the details follow.
The adjustment for favorable selection is made by taking the ratio of the average risk factor of managed care enrollees to the average risk factor of FFS Medicare beneficiaries in each county. The risk factor is calculated by CMS for each Medicare eligible and is the ratio of that eligible's expected spending to the average spending of Medicare beneficiaries. The calculation of the risk factor and the model of spending it is based on until 2003 are described in detail in Ingber (2000) and Pope et al. (2000). Briefly, CMS predicts spending as a function of each beneficiary's demographics and inpatient diagnoses (if available) for the previous years.
As Greenwald et al. (2000) point out, the ratio of the average risk factor of managed care enrollees to the average risk factor of FFS Medicare beneficiaries may therefore serve as a measure of the amount of favorable selection that Medicare managed care plans experience, as it is an estimate of the ratio of managed care enrollees' spending to FFS Medicare beneficiaries' spending. Greenwald et al. (2000) cite their finding that the risk factors of Medicare HMO enrollees are lower on average than those of beneficiaries in FFS Medicare as evidence for favorable selection in the Medicare managed care program.
Table 7 shows the mean average risk factors separately for both HMO enrollees and FFS beneficiaries (where the mean is calculated across counties with Medicare managed care plans and weighted by the Medicare eligible population) and the mean ratio of the average risk factor of HMO enrollees to average risk factor of FFS beneficiaries for the years 1999 through 2001. The data on risk factors of Medicare beneficiaries for 2002 were not available. As the table shows, from 1999 to 2001, the mean average risk factor for Medicare HMO enrollees in these counties was about .9 and the mean average risk factor for Medicare FFS beneficiaries was about .97, making the ratio of the two just above .9. In other words, the average Medicare HMO enrollee had a risk profile such that they were expected to cost just over 90% as much as the average Medicare FFS beneficiary.
Table 8 shows the calculation of counterfactual Medicare FFS spending adjusting for favorable selection using the ratios of the risk factors for the two categories of Medicare beneficiaries. As part of the process for setting reimbursement rates for Medicare private plans, CMS reports the average monthly spending of Medicare FFS beneficiaries for each county and year. The first row of the table shows the mean of these averages across counties for each year (deflated to 2000 levels with the GDP deflator and weighted by Medicare-eligible population); this figure rises from $467 in 1999 to $558 in 2002. The second row shows the total number of Medicare HMO enrollees in each year. The third row shows total potential annual spending in the FFS program of these enrollees not adjusted for selection, found by multiplying the average FFS spending in each county by the number of HMO enrollees in that county and aggregating over counties. This figure rises from about $35 billion in 1999 to $37 billion in 2000 and then drops to $33 billion in 2002, as the number of Medicare HMO enrollees drops.
The adjustment for selection is then applied by multiplying the average FFS spending by the ratio of the risk factors separately in each county to give an estimate of what would have been spent on a Medicare HMO enrollee in the FFS program. The fourth line of the table reports the mean ratio of the average risk factor for Medicare HMO enrollees to the average risk factor for FFS beneficiaries. As noted above, data on risk factors were not available for 2002, however. In order to calculate net costs for 2002, I attribute the ratio for 2001 for each county to the same county in 2002. (I use the ratio from 2000 or 1999, if a county is present in the data for one of those years and 2002, but not 2001; for the few remaining counties that enter the data for the first time in 2002, I use the average in 2001 for other counties in the same state.) The fifth line of the table reports the mean of the adjusted average FFS spending across counties (and weighted by Medicare-eligible population); average monthly counterfactual spending on Medicare HMO enrollees adjusted for selection rises from $422 in 1999 to $515 in 2002.
The last row of the table aggregates this average monthly spending over counties to give total counterfactual spending on Medicare HMO enrollees in the FFS program in each year; this figure rises from about $32 billion in 1999 to $34.3 billion in 2000, before dropping to $30.8 billion in 2002.
Table 9 puts together the calculations in Tables 7 and 8 to give a calculation of the net cost of the Medicare managed care program in 1999-2002. The first line shows the annual actual spending on the Medicare HMO program as calculated in Table 7 and the second line gives the annual counterfactual spending by the Medicare FFS program on Medicare HMO enrollees if they had been enrolled in the Medicare FFS program as calculated in Table 8. The last line gives the difference, which is the net cost of the program. The annual net cost hovers around $6 billion from 1999 to 2001 and then drops to just over $2 billion in 2002. Net costs drop in 2002 because actual spending on the Medicare HMO program fell considerably more than counterfactual spending in that year. The calculation of counterfactual spending, however, partly rests on the assumption that the mean ratio of the average risk factor of HMO enrollees to that of FFS beneficiaries was about the same as in earlier years. Since payments to HMOs were partly adjusted with the risk factor, however, the lower actual spending may reflect increased favorable selection in the Medicare HMO program in 2002 which, in turn, would suggest lower counterfactual spending and higher net costs of the program than what is shown in Table 8. In the absence of data on risk factors for 2002, however, I will merely note that the results on costs for that year are less reliable than those for the other three years.
9 Net welfare of the Medicare HMO program and the return on government spending on the program in 1999-2002
Table 10 combines the results of the welfare analysis as reported in Table 5 and the calculations of the net cost in Table 9 to give an estimate of the net welfare provided by and the return on government spending on the Medicare managed care program from 1999 to 2002. The net welfare (reported in the third line of Table 10) is the net cost (reported in the second line) subtracted from the gross aggregate welfare (reported in the first line). The annual return on spending (reported in the fourth line) is simply the annual net welfare divided by the annual net cost. The net welfare is estimated to be between $10 and $11 billion in 1999 and 2000; this estimate drops to about $8 billion in 2001, and rises back up to $10 billion in 2002. The return on government spending is measured to be 159% in 1999; in other words, the program provides more than two and a half times as much welfare as it costs the government. This figure rises to 176% in 2000, then drops to 129% in 2001 before ballooning to 451% in 2002, as net costs of the program drop sharply that year while welfare provided by the program does not fall as much. As noted in the previous section, however, the calculation of the net costs for 2002 are less reliable than for the other years in the table and actual net costs may, in fact, be higher, so the return on spending on the Medicare HMO program in 2002 may, in reality, be more in line with those of the first three years.
The last column reports the totals for the four-year period. Total gross welfare provided by the program from 1999 to 2002 was $60.8 billion and total net costs during this time were about $21.3 billion, yielding a return on spending on the program of about 186%. In other words, during this period, the program provides nearly three times as much welfare as it cost. If we do the same calculation for the three years for which there are reliable data on favorable selection in the Medicare HMO program, total gross welfare is $48.3 billion and total net costs are around $19 billion, giving a return of about 155% on government spending on the program.
10 Conclusion
The Medicare managed care program has caused some controversy because the program was originally intended to lower the costs of the Medicare program but has only raised them. Many view the plans participating in the program as overpaid and there have been many calls for cuts in the plan's payment rates. On the other hand, previous cuts in the program that were passed in 1997 caused a substantial protest from many Medicare beneficiaries and ended up being rescinded in 2003.
As noted in the quote at the beginning of this paper, it is important to measure the benefits of the program as well as the costs. In this paper, I estimate the welfare provided by the program in the period 1999 through 2002 by estimating demand for Medicare HMO premiums and benefits in a model where the HMOs are treated as differentiated products. I also calculate the net costs of the program in this period by subtracting counterfactual costs of the Medicare HMO enrollees from actual spending on the program; the counterfactual costs are calculated based on average FFS costs in each county adjusted for favorable selection in the Medicare HMO program. I find that the program provided nearly $61 billion in consumer surplus while costing the government, on net, about $21 billion in the years 1999 through 2002 and therefore gave a return on government spending of about 186% during this period. The program was clearly "worth it" since it gave a positive return on spending, and the return is substantial when compared to returns on private investment.
Policymakers may wish to take this return on spending into account when deciding reimbursement policy for the program. These results come with several caveats, however. First, they only apply to HMOs as that was the only type of plan involved in the program during the years 1999 through 2002. There is evidence suggesting that the other types of plans that have entered the program since then, such as private fee-for-service plans, are less cost-effective (Medicare Payment Advisory Commission 2008). In addition, these results apply only to the period 1999 through 2002, as that was the only period for which I was able to obtain detailed data on plan benefits, and as the changes to the Medicare Advantage program made since then have an ambiguous effect on the return on government spending. The Medicare Modernization Act, passed in 2003, raised payment rates for plans, and this raise, in turn, triggered more plans' entry into the program and induced them to offer more generous benefits, with the result that enrollment in the Medicare Advantage program, as a percentage of total Medicare enrollment, returned to the level of its peak of 1999 in 2006. On the one hand, the payment rates for private plans in each county were increased to at least 100% of per capita FFS expenditures in the same county. This increase would almost certainly raise the net cost of the program as it is highly unlikely that the ratio of private plan enrollees' costs to those of FFS beneficiaries would have risen above one, even though private plan enrollment increased as a share of total Medicare enrollment. On the other hand, the entry of plans into the program and more generous benefits would raise the welfare generated by the program. Recently, the plans' payment rates were cut again, which may have effects on entry and plan benefits opposite to those of the Medicare Modernization Act. Without data on the benefits being offered, however, it is not possible to estimate the return on government spending for the Medicare Advantage program currently.
Arellano, M. Computing robust standard errors for within-groups estimators. Oxford Bulletin of Economics and Statistics 1987; 49 (4); 431-434.
Atherly A, Dowd B E, Feldman R. The effect of benefits, premiums, and health risk on health plan choice in the Medicare program. Health services research 2004; 39 (4, Part I); 847-864.
Banthin J S, Taylor A K. Research Findings #15: HMO enrollment in the United States, household reported estimates, 1996. Agency for Healthcare Research and Quality. 2001.
Berry S T. Estimating discrete-choice models of product differentiation. The RAND Journal of Economics 1994; 25 (2); 242-262.
Biles B, Nicholas L H, Cooper B S, Adrion E, Guterman S. The cost of privatization: extra payments to Medicare Advantage plans-updated and revised. The Commonwealth Fund. 2006.
Brown R S, Clement D G, Hill J W, Retchin S M, Bergeron J W. Do health maintenance organizations work for Medicare?. Health Care Financing Review 1993; 15 (1); 7-23.
Cox D F, Hogan C. Biased selection and Medicare HMOs: analysis of the 1989-1994 experience. Medical Care Research and Review 1997; 54 (3); 259-274.
General Accounting Office. Medicare: issues raised by Florida health maintenance organizations: report to Congress. 1986.
Greenwald L M, Levy J M, Ingber M J. Favorable selection in the Medicare+Choice program: new evidence. Health care financing review 2000; 21 (3), 127-134.
Hausman J A. Valuation of new goods under perfect and imperfect competition. In: Bresnahan T F (Ed), The economics of new goods, Vol. 58 of NBER studies in income and wealth. University of Chicago Press: Chicago; 1997. p. 207-248.
Ingber M J. Implementation of risk adjustment for Medicare. Health care financing review 2000; 21 (3); 119-126.
Kaiser Family Foundation. Medicare Chartbook. 2005.
Medicare Payment Advisory Commission. Report to the Congress: Medicare payment policy. 2008.
Mello M M, Stearns S C, Norton E C, Ricketts T C. Understanding biased selection in Medicare HMOs. Health services research 2003; 38 (3); 961-992.
Morgan R O, Virnig B A, DeVito C A, Persily N A. The Medicare-HMO revolving door - the healthy go in and the sick go out. The New England Journal of Medicine 1997; 337 (3); 169-175.
Neuman P, Cubanski J, Desmond K A, Rice T H. How much skin in the game do Medicare beneficiaries have? The increasing burden of health care spending, 1997-2003. Health Affairs 2007; 26 (6); 1692-1701.
Nevo A. Measuring market power in the ready-to-eat cereal industry. Econometrica 2001; 69 (2); 307-342.
Orszag, P. Statement of Peter R. Orszag, Director, Congressional Budget Office: The Medicare Advantage program: trends and options, before the subcommittee on health, Committee on Ways and Means, U.S. House of Representatives. 2007.
Pope G C, Ellis R P, Ash A S, Liu C-F, Ayanian J Z, Bates D W, Burstin H, Iezzoni L I, Ingber M J. Principal inpatient diagnostic cost group model for Medicare risk adjustment. Health Care Financing Review 2000; 21 (3); 93-118.
Small K A, Rosen H S. Applied welfare economics with discrete choice models. Econometrica 1981; 49 (1); 105-130.
Thiede K, Dowd B, Feldman R, Jaciejewski M. Selection experience in Medicare HMOs: pre-enrollment expenditures. Health Care Financing Review 1999; 20 (4); 197-209.
Town R, Liu S. The welfare impact of Medicare HMOs. The RAND Journal of Economics 2003; 34 (4); 719-736.
Zarabozo C. Milestones in Medicare managed care. Health Care Financing Review 2000; 22 (1); 61-67.
| Year | 1999 | 2000 | 2001 | 2002 |
| Number of Medicare HMO Contracts | 280 | 257 | 169 | 139 |
| Number of counties with Medicare HMOs | 794 | 752 | 601 | 540 |
| Number of HMO-county combinations | 1,924 | 1,790 | 1,175 | 954 |
| Mean Medicare HMO market share | 10.2% | 10.7% | 12.5% | 13.4% |
| Mean enrollment in a HMO-county combination | 3,150 | 3,444 | 4,649 | 5,069 |
| Mean market share of FFS Medicare | 74.9% | 74.6% | 75.4% | 76.2% |
| Mean number of Medicare HMOs | 2.42 | 2.38 | 1.97 | 1.77 |
a Deflated to 2000 levels by the CPI for all items.
b Deflated to 2000 levels by the CPI for prescription drugs.
| Year | 1999 | 2000 | 2001 | 2002 |
| Number of HMO-county combinations | 1,924 | 1,790 | 1,175 | 954 |
| Mean monthly premiuma | $11.55 | $21.45 | $29.95 | $37.01 |
| Percent of plans offering prescription drug benefits | 73.1% | 66.9% | 51.7% | 51.8% |
| Percent of plans offering brand-name drug coverage | 69.4% | 64.5% | 43.5% | 34.7% |
| Mean brand-name drug coverage limitb | $702.76 | $480.39 | $381.90 | $252.89 |
| Mean co-payment for primary care visita | $7.68 | $8.75 | $9.71 | $10.38 |
| Mean co-payment for visit to specialista | $8.54 | $10.50 | $12.52 | $15.11 |
| Mean inpatient deductiblea | $20.61 | $41.08 | $80.45 | $132.31 |
| Percent of plans not requiring a referral to see a specialist | 1.3% | 1.3% | 1.9% | 6.9% |
| Percent of plans offering vision coverage | 92.7% | 89.8% | 86.6% | 85.4% |
| Percent of plans offering dental coverage | 32.3% | 19.3% | 23.4% | 14.2% |
a Deflated to 2000 levels by the CPI for all items. a Deflated to 2000 levels by the CPI for all items. a Deflated to 2000 levels by the CPI for all items. a Deflated to 2000 levels by the CPI for all items. a Deflated to 2000 levels by the CPI for all items.
b Deflated to 2000 levels by the CPI for prescription drugs. b Deflated to 2000 levels by the CPI for prescription drugs. b Deflated to 2000 levels by the CPI for prescription drugs. b Deflated to 2000 levels by the CPI for prescription drugs. b Deflated to 2000 levels by the CPI for prescription drugs.
| (1) Logit | (2) Two-level nested logit | (3) Three-level nested logit | (4) Logit | (5) Two-level nested logit | (6) Three-level nested logit | |
| Premium | -0.006 | -0.007 | -0.007 | -0.005 | -0.007 | -0.007 |
| Premium Standard Error | (-0.001) | (0.001) | (0.001) | (0.001) | (0.001) | (0.001) |
| Dummy for prescription drug benefits | 0.086 | 0.091 | 0.058 | |||
| Dummy for prescription drug benefits Standard Error | (0.030) | (0.032) | (0.030) | |||
| Prescription drug benefits: Monthly brand-name drug coverage amount in $100s | 0.148 | 0.165 | 0.126 | |||
| Prescription drug benefits: Monthly brand-name drug coverage amount in $100s Standard Error | (0.036) | (0.036) | (0.037) | |||
| Prescription drug benefits: Monthly brand-name drug coverage amount in $100s squared | -0.010 | -0.012 | -0.009 | |||
| Prescription drug benefits: Monthly brand-name drug coverage amount in $100s squared Standard Error | (0.003) | (0.003) | (0.003) | |||
| Prescription drug benefits: Dummy for generic coverage | -0.044 | 0.032 | -0.061 | |||
| Prescription drug benefits: Dummy for generic coverage Standard Error | (0.035) | (0.041) | (0.035) | |||
| Nondrug benefits: Co-payment for visit to primary care doctor in $1s | -0.014 | -0.012 | -0.007 | |||
| Nondrug benefits: Co-payment for visit to primary care doctor in $1s Standard Error | (0.004) | (0.004) | (0.004) | |||
| Nondrug benefits: Co-payment for visit to specialist in $1s | -0.001 | -0.003 | -0.003 | |||
| Nondrug benefits: Co-payment for visit to specialist in $1s Standard Error | (0.002) | (0.002) | (0.002) | |||
| Nondrug benefits: Inpatient deductible in $100s | -0.010 | -0.008 | -0.014 | |||
| Nondrug benefits: Inpatient deductible in $100s Standard Error | (0.005) | (0.005) | (0.005) | |||
| Nondrug benefits: Plan does not require referral to see specialist | 0.183 | 0.264 | 0.247 | |||
| Nondrug benefits: Plan does not require referral to see specialist Standard Error | (0.072) | (0.076) | (0.077) | |||
| Nondrug benefits: Plan offers vision benefits | 0.049 | -0.008 | 0.093 | |||
| Nondrug benefits: Plan offers vision benefits Standard Error | (0.039) | (0.042) | (0.039) | |||
| Nondrug benefits: Plan offers dental benefits | 0.100 | 0.075 | 0.048 | |||
| Nondrug benefits: Plan offers dental benefits Standard Error | (0.029) | (0.029) | (0.030) | |||
| Log(plan share | group share) | 0.009 | 0.228 | 0.345 | 0.515 | ||
| Log(plan share | group share) Standard Error | (0.107) | (0.110) | (0.092) | (0.103) | ||
| Log(group share | HMO share) | 0.280 | 0.531 | ||||
| Log(group share | HMO share) Standard Error | (0.101) | (0.096) | ||||
| Observations | 5,851 | 5,851 | 5,851 | 5,851 | 5,851 | 5,851 |
Dependent variable: Log(plan market share) - log(traditional Medicare market share)
Notes: All regressions include year effects and plan-county fixed effects. Robust standard errors are reported in parentheses and are calculated by the formula for fixed-effects estimators given in Arellano (1987). Market shares for plans and for traditional Medicare have been adjusted to reflect that beneficiaries enrolled in Medicaid or an employer-sponsored supplemental retirement plans are not counted among those eligible for a Medicare HMO. Premium, log(plan share | group share), and log(group share | HMO share) are instrumented. Instruments for premium include the weighted average of competitors' premiums in other counties in the plan's service area and the county reimbursement rate. The instruments for log(plan share | group) are the average covered drug expenditure and the averages of the nondrug benefits of other plans in the same drug/nondrug group. The instruments for log(group share | HMO) are the average covered drug expenditure and the averages of the nondrug benefits of plans in the other drug/nondrug group in the same county. The premiums, co-payments, and deductibles were deflated to 2000 levels with the CPI for all items. The brand-name drug coverage amount was deflated to 2000 levels with the CPI for prescription drugs.
| (1) Logit | (2) Two-level nested logit | (3) Three-level nested logit | |
| Drug benefits: Prescription drug benefit | $15.28 | $13.63 | $7.99 |
| Drug benefits: Prescription drug benefit Standard Errors | ($-5.85) | ($-4.79) | ($-4.30) |
| Drug benefits: First $100 of brand-name drug coverage | $29.24 | $22.89 | $17.78 |
| Drug benefits: First $100 of brand-name drug coverage Standard Errors | ($-10.83) | ($-6.99) | ($-6.42) |
| Drug benefits: Generic drug coverage | -$9.29 | $4.81 | -$9.31 |
| Drug benefits: Generic drug coverage Standard Errors | ($-8.36) | ($-5.83) | ($-5.97) |
| Nondrug benefits: Reduce co-payment for visit to primary care doctor by $1 | $3.14 | $2.04 | $1.08 |
| Nondrug benefits: Reduce co-payment for visit to primary care doctor by $1 Standard Errors | ($-1.35) | ($-0.76) | ($-0.67) |
| Nondrug benefits: Reduce co-payment for visit to specialist by $1 | $0.41 | $0.53 | $0.54 |
| Nondrug benefits: Reduce co-payment for visit to specialist by $1 Standard Errors | ($-0.48) | ($-0.33) | ($-0.33) |
| Nondrug benefits: Reduce inpatient deductible by $100 | $2.19 | $1.29 | $2.12 |
| Nondrug benefits: Reduce inpatient deductible by $100 Standard Errors | ($-1.32) | ($-0.85) | ($-0.87) |
| Nondrug benefits: Remove requirement for referral before seeing specialist | $41.51 | $38.71 | $37.97 |
| Nondrug benefits: Remove requirement for referral before seeing specialist Standard Errors | ($-18.91) | ($-12.77) | ($-12.93) |
| Nondrug benefits: Dental benefits | $22.66 | $12.20 | $8.17 |
| Nondrug benefits: Dental benefits Standard Errors | ($-9.13) | ($-5.26) | ($-4.89) |
| Nondrug benefits: Vision benefits | $12.13 | $2.59 | $15.10 |
| Nondrug benefits: Vision benefits Standard Errors | ($-9.41) | ($-6.36) | ($-6.71) |
Note: Based on estimates in Table 3.
| Year | 1999 | 2000 | 2001 | 2002 |
| Mean monthly welfare per Medicare eligible (2000 $)a | $ 84.58 | $ 86.31 | $ 80.19 | $ 71.45 |
| Mean monthly welfare per Medicare eligible (2000 $)a Bootstrapped standard errors | ($14.29) | ($14.81) | ($14.02) | ($13.06) |
| Number of Medicare beneficiaries eligible for a Medicare HMO (millions) | 16.5 | 16.3 | 15.3 | 14.6 |
| Aggregate annual welfare (2000 $ billions) | $16.7 | $16.9 | $14.7 | $12.5 |
| Aggregate annual welfare (2000 $ billions) Bootstrapped standard errors | ($2.6) | (-2.6) | (-2.3) | (-1.9) |
Notes: Bootstrapped standard errors are reported in parentheses. The number of Medicare beneficiaries in HMO counties has been adjusted to reflect that beneficiaries enrolled in Medicaid or an employer-sponsored supplemental retirement plans are not counted among those eligible for a Medicare HMO.
a Weighted by Medicare population
| Year | 1999 | 2000 | 2001 | 2002 | 2003 |
| Amount spent on the Medicare HMO program (fiscal year basis, nominal $ billions)a | n.a. | 39.8 | 42.0 | 33.8 | 36.4 |
| Amount spent on the Medicare HMO program (calendar year basis, 2000 $ billions)b | n.a. | 40.4 | 39.0 | 33.1 | |
| Total reimbursements to Medicare HMOs (2000 $ billions) | 36.5 | 38.2 | 36.2 | 32.3 | |
| Percent spent on administrationc | 5.3% | 5.6% | 7.9% | 2.4% | |
| Amount spent on the Medicare HMO program (2000 $ billions) | 38.4d | 40.4 | 39.0 | 33.1 |
a Taken from CMS's financial statements for fiscal years 2000-2003
b Weighted average of the amounts on the financial statements, with the same fiscal year receiving a three-quarters weight and the following fiscal year receiving a one-quarter weight. Deflated by the GDP deflator
c This percentage was calculated by dividing the total amounts spent on the program in 2000-2002 by the total reimbursements. Since the financial statement for 1999 was not available, the percentage for 1999 is an average of the three following years.
d This amount was calculated by adding the estimated percent spent on administration to the total reimbursements in 1999.
| Year | 1999 | 2000 | 2001 |
| Mean average risk factor for Medicare HMO enrolleesa | 0.88 | 0.89 | 0.90 |
| Mean average risk factor for Medicare FFS beneficiariesa | 0.97 | 0.97 | 0.97 |
| Mean ratio of Medicare HMO average risk factor to Medicare FFS average risk factora | 0.91 | 0.92 | 0.92 |
a Weighted by Medicare population.
| Year | 1999 | 2000 | 2001 | 2002 |
| Mean average monthly per capita FFS spending in Medicare HMO counties (2000 $)a | $467.25 | $488.05 | $520.55 | $557.73 |
| Number of Medicare HMO enrollees (millions) | 6.1 | 6.2 | 5.5 | 4.9 |
| Total potential annual FFS spending on Medicare HMO enrollees, unadjusted for selection (2000 $ billions) | 35.1 | 37.2 | 35.3 | 33.3 |
| Average ratio of Medicare HMO risk factor to Medicare FFS risk factor | 0.91 | 0.92 | 0.92 | 0.92b |
| Mean average monthly per capita FFS spending in Medicare HMO counties, adjusted for selection (2000 $) | $422.30 | $447.21 | $479.35 | $514.64 |
| Total potential annual FFS spending on Medicare HMO enrollees, adjusted for selection (2000 $ billions) | 32.0 | 34.3 | 32.6 | 30.8 |
a Weighted by Medicare population.
b The average risk factors for each county in 2001 have been attributed to 2002, since data for 2002 were not available. If the county was not present in the 2001 data, the average risk factor for 2000 or 1999 was used. If the county was not previously present in the data in any year, the average ratio in 2001 for the state in which the county was located was attributed to the county.
| Year | 1999 | 2000 | 2001 | 2002 |
| Actual spending on the Medicare HMO program | 38.4 | 40.4 | 39.0 | 33.1 |
| Counterfactual Medicare FFS spending on managed care enrollees | 32.0 | 34.3 | 32.6 | 30.8 |
| Net cost of Medicare HMO program | 6.5 | 6.1 | 6.4 | 2.3 |
| Year | 1999 | 2000 | 2001 | 2002 | Total |
| Aggregate welfare | 16.7 | 16.9 | 14.7 | 12.5 | 60.8 |
| Net cost | 6.5 | 6.1 | 6.4 | 2.3 | 21.3 |
| Net welfare | 10.3 | 10.8 | 8.3 | 10.3 | 39.6 |
| Return on program | 159.1% | 176.2% | 129.4% | 450.7% | 186.3% |