FEDS Notes
August 05, 2022
Long COVID, Cognitive Impairment, and the Stalled Decline in Disability Rates
Brendan M. Price
Introduction
Long COVID encompasses a suite of long-term symptoms that commonly include fatigue, shortness of breath, and so-called brain fog, along with many others. Individuals with long-term symptoms may be unable to work (or work full-time) as a result of their condition, and there is growing evidence that long COVID may be restraining labor supply.1
In this note, I use two survey datasets to document four facts about long COVID in the United States. First, long-term COVID symptoms are much more prevalent among women, adults under 65, Hispanics and Latinos, and non–college graduates than among other demographic groups. Second, COVID "long haulers" cite specific physical and cognitive impairments commonly associated with the condition in media and medical reporting. Third, the share of working-age adults reporting serious difficulty remembering, concentrating, or making decisions has risen steadily since the start of the pandemic. Fourth, growing shares of women and of non–college graduates report simultaneously (i) being out of the labor force due to disability and (ii) experiencing these cognitive difficulties. Non-participation attributed to disability was declining steadily in the years leading up to the pandemic, but that downward trend has stalled. Long COVID is likely one reason why.
I. Evidence from the Household Pulse Survey
Newly available data from the Household Pulse Survey—an experimental Census Bureau product launched at the start of the pandemic—provide the first large-scale, population-level detail on the prevalence of long COVID.2 Starting with the survey's June 2022 wave, respondents who report having had a diagnosed case of COVID are asked,
"Did you have any symptoms lasting 3 months or longer that you did not have prior to having coronavirus or COVID-19?"
Though there is no universally agreed-upon definition of long COVID, the three-month threshold is a common criterion. To aid responses to this question, the survey questionnaire provides a list of symptoms frequently associated with long COVID.3
The Pulse Survey suffers from an extremely low response rate, around 6 percent in recent survey waves. In addition, respondents cannot be linked over time, precluding longitudinal analyses that would facilitate causal inference about the effects of long COVID. For these reasons, the Pulse data may be more useful as a barometer of qualitative patterns than as a reliable gauge of magnitudes. With these caveats noted, I use the June and July 2022 survey waves to estimate the prevalence of long COVID and its associated impairments.4
The prevalence of long COVID
Among adults aged 18 or older, 41 percent of Pulse respondents report having been diagnosed with COVID at some point in the past; 14 percent of all respondents, and 35 percent of those with diagnosed COVID, report having experienced symptoms lasting three or more months. The prevalence of long COVID in the Pulse data is roughly in line with some external estimates that about 30 percent of COVID patients go on to develop long COVID.5 Just over half of long haulers report that they are currently experiencing symptoms.
The incidence of long COVID varies greatly across demographic groups. As shown in Figure 1, long COVID is significantly more common among women, among individuals under 65, among Hispanics and Latinos, and among those without a college education.6 I return to disparities by gender and educational attainment later in my analysis.
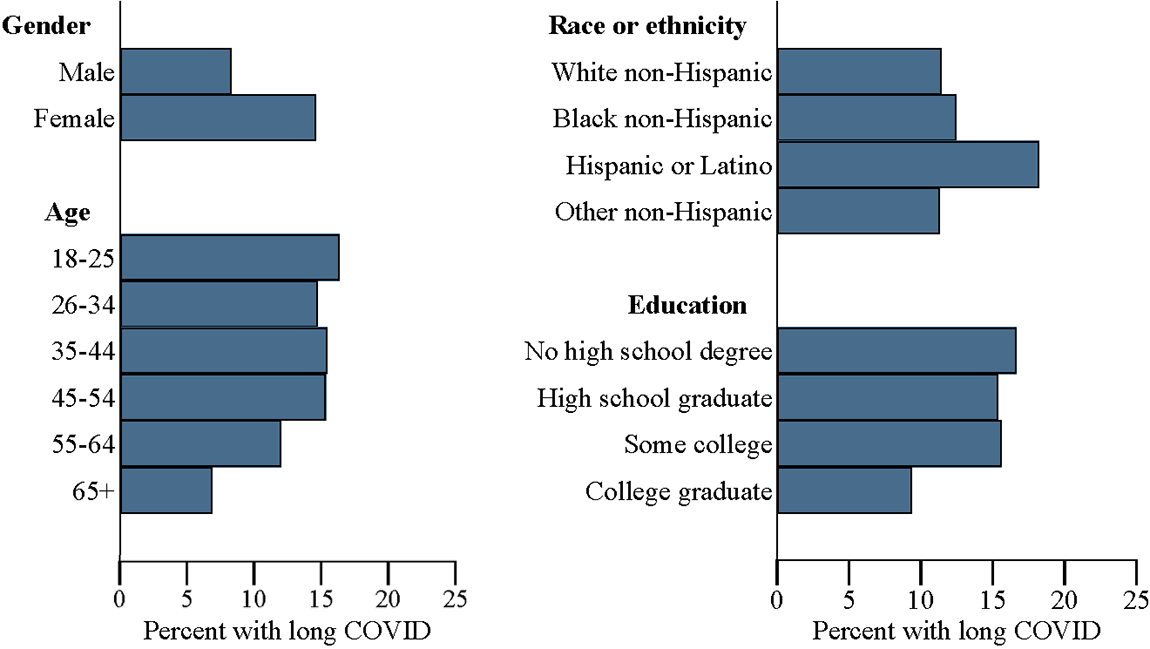
Note: This and all subsequent exhibits use sampling weights to obtain representative estimates.
Source: Census Household Pulse Survey and author’s calculations.
The rest of this note focuses on adults aged 18–64, for whom long COVID is much more common than for seniors.
Symptoms of long COVID
The Pulse survey also asks a set of questions about physical and cognitive impairment. Figure 2 shows the share of respondents who express "a lot" of difficulty with a given activity (the darker portion of each bar) or at least "some" difficulty (the full height of each bar), separately by long COVID status. Consistent with medical and media reports, long haulers are much more likely to cite difficulties remembering or concentrating, walking or climbing stairs, and dressing or bathing than other adults do.
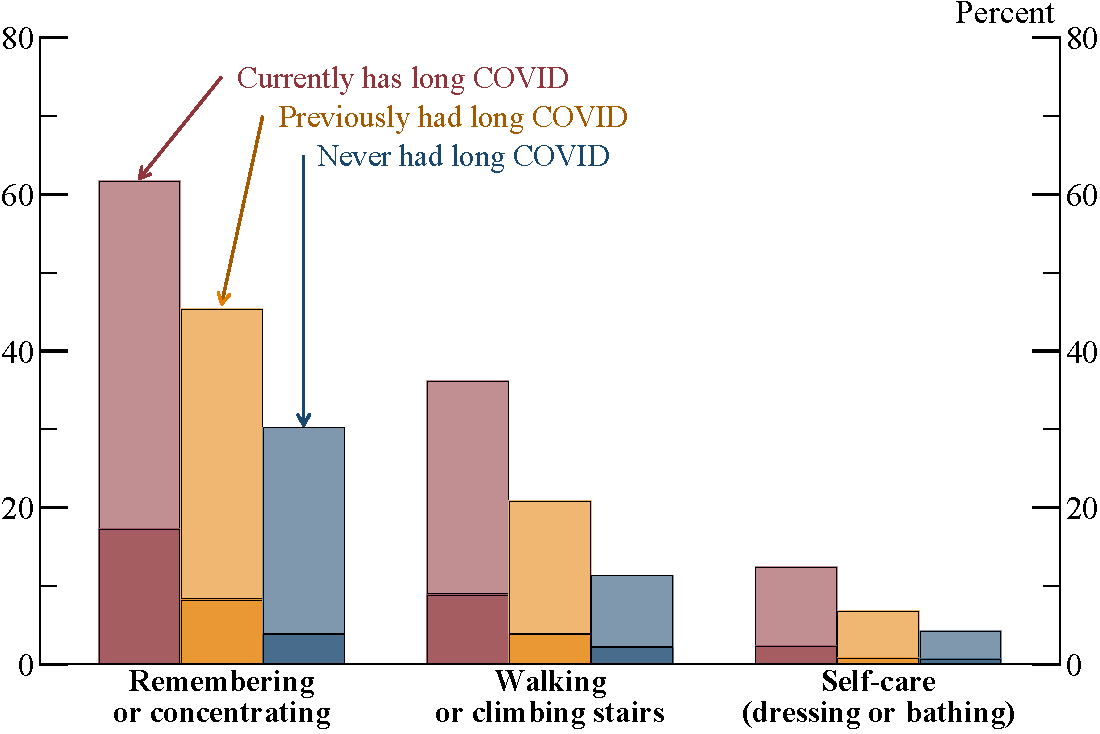
Note: Sample is restricted to ages 18–64. Dark portion of each bar (beneath the horizontal line) indicates “a lot” of difficulty; light portion of each bar (above the horizontal line) indicates “some” difficulty.
Source: Census Household Pulse Survey and author’s calculations.
A degree of cognitive difficulty is especially common, cited by 62 percent of adults who currently report long-term COVID symptoms compared with 30 percent of those who have never had long-term symptoms.7 Such difficulty is also elevated among those whose long-term symptoms have ostensibly resolved, either because of subjectivity in self-reported long COVID status or because long haulers are in worse health partly for reasons unrelated to the coronavirus.
Long haulers also report high rates of psychological distress: for example, 38 percent felt down, depressed, or hopeless more than half of the days in the preceding two weeks, compared with 16 percent of adults who never had long COVID. Similar patterns hold for survey questions about anxiety, worry, and little interest or pleasure in doing things.
Possible effects on employment
Long-term COVID symptoms appear to significantly interfere with daily activities for many who suffer from them. Previous research on the labor market effects of medical and psychological impairments suggests that these symptoms are likely to constrain labor supply, as well.8
The Pulse survey asks questions about employment status and reasons for non-employment, and in unreported regressions I explore the relationship between employment and long COVID. Controlling for available demographics, I find that individuals who have had long COVID are about 3 percentage points less likely to be employed than those who had COVID but did not experience symptoms lasting more than three months. Individuals with long COVID are also more likely to report being out of work because they are sick with COVID or caring for someone sick with COVID. However, these cross-sectional relationships are likely to be biased by unobservable differences in underlying health status and labor market attachment. For that reason, regression estimates using the Pulse data are suggestive at best, and I do not pursue them further.
II. Evidence from the Current Population Survey
The Pulse survey has important shortcomings, including a low response rate, a modest sample size, and a lack of pre-pandemic history. To put the pandemic period into a broader context, and to ground my analysis in a larger and more representative dataset, I use Current Population Survey (CPS) data from IPUMS on adults aged 18–64, spanning January 2017 through June 2022 (Flood et al., 2021).
Impairments consistent with long COVID
The CPS lacks a question about long COVID, but it does contain a set of questions about physical and cognitive impairments similar to those asked in the Household Pulse Survey. Consistent with the evidence from Pulse, Figure 3 shows that the share of working-age adults who report "serious" difficulty remembering, concentrating, or making decisions has risen 0.6 percentage point since February 2020. Other forms of impairment—difficulty walking or climbing stairs, running errands, and dressing or bathing—are also elevated above their pre-pandemic trends.
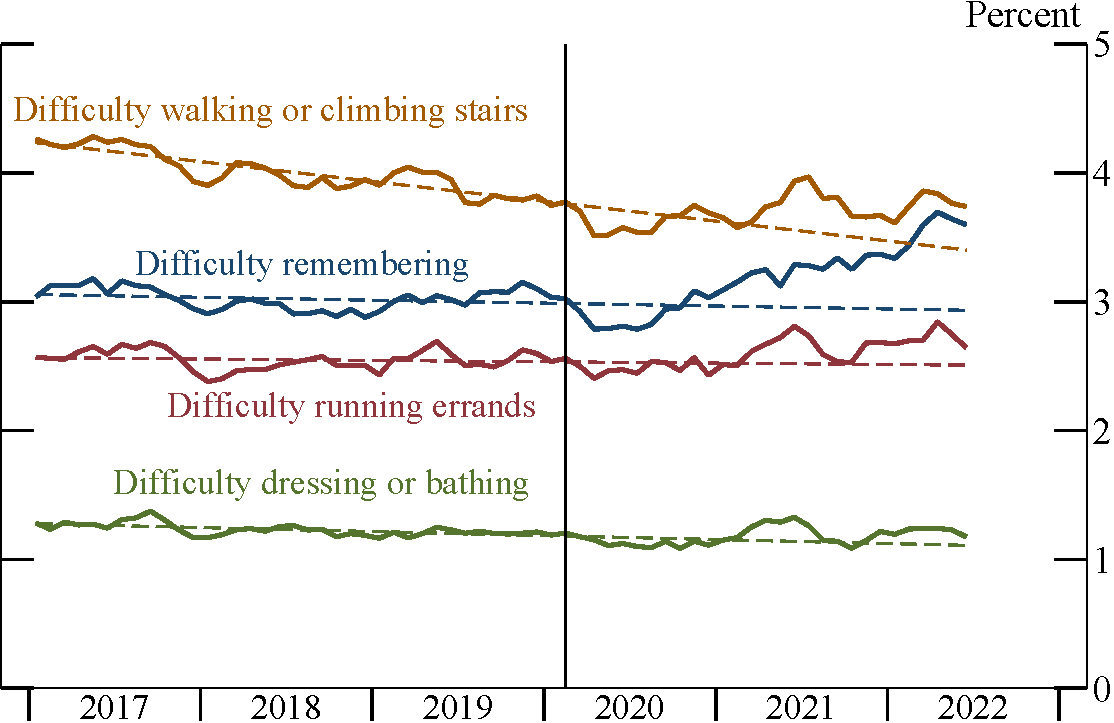
Note: Sample is restricted to ages 18–64. Vertical bar indicates February 2020. Dashed lines are extrapolations of 2017–19 trends.
Source: Current Population Survey and author’s calculations.
The Pulse data indicate that women and those without a college degree are especially likely to have long COVID. The CPS corroborates this point. As shown in Figure 4, the shares of women and non–college graduates who report serious cognitive difficulties have risen especially sharply over the course of the pandemic.
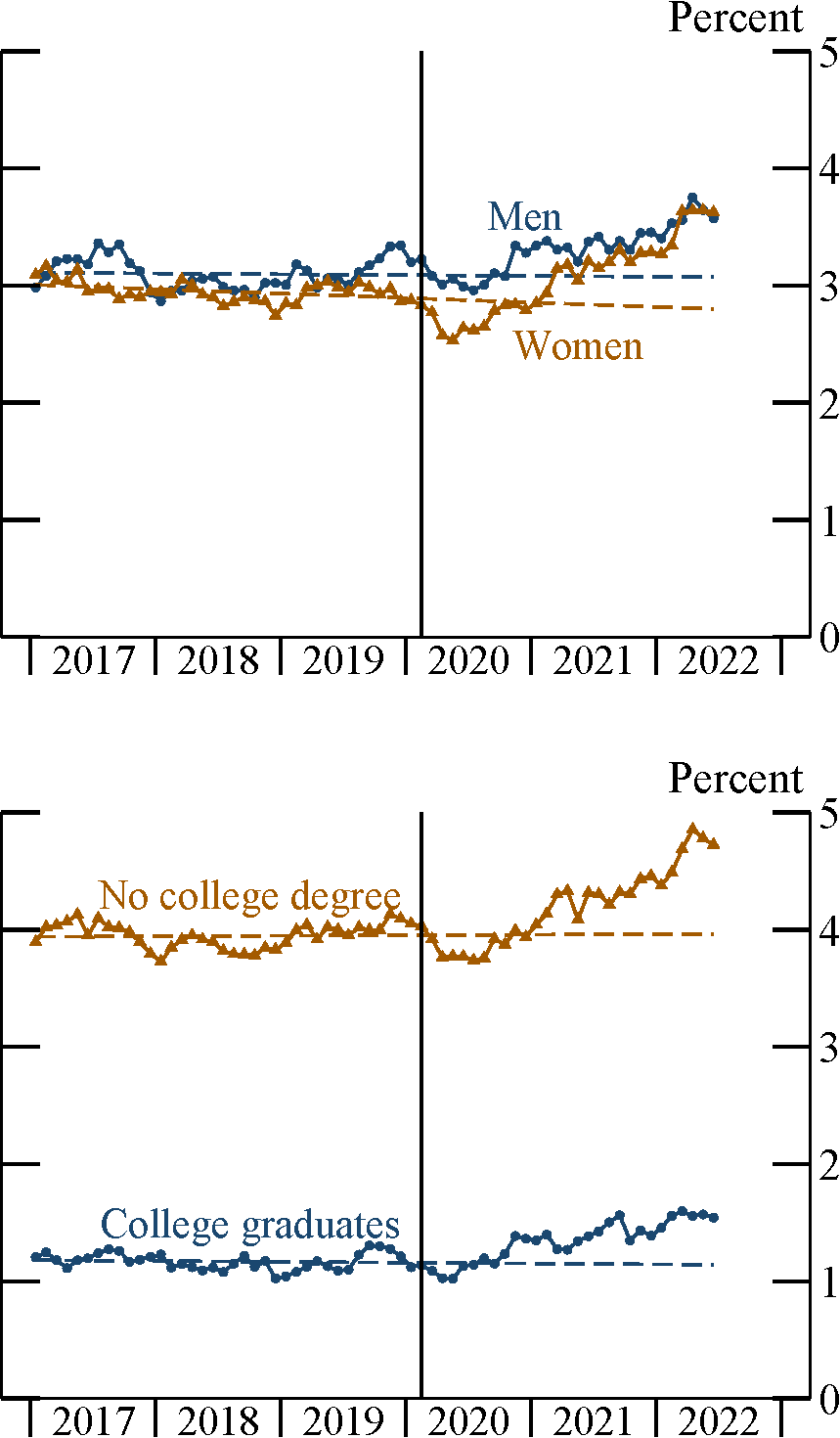
Note: Sample is restricted to ages 18–64. Vertical bar indicates February 2020. Dashed lines are extrapolations of 2017–19 trends.
Source: Current Population Survey and author’s calculations.
Non-participation due to disability
The CPS asks respondents who are not in the labor force their primary reason for non-participation. As shown in Figure 5, the share of working-age adults out of the labor force due to disability, illness, or inability to work was in secular decline in the years preceding the pandemic, but—after a short-lived decline in 2020—has been holding relatively steady for the past two years.9 As of June 2022, this share is 0.6 percentage point above its pre-pandemic trend.
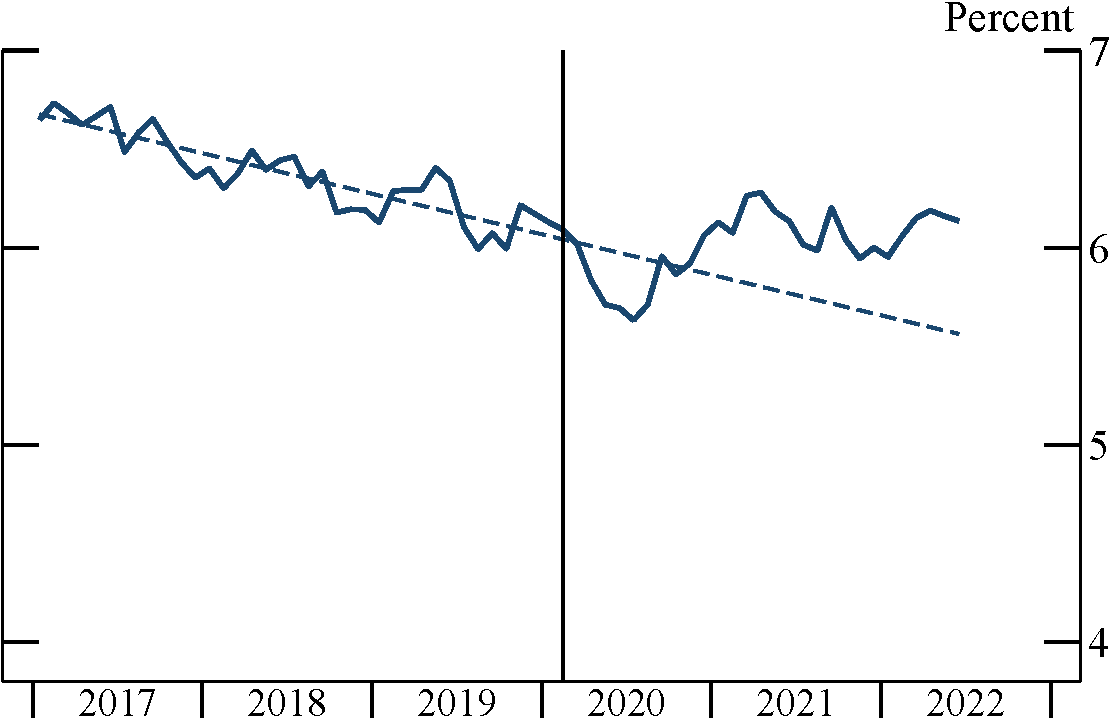
Note: Sample is restricted to ages 18–64. Vertical bar indicates February 2020. Dashed lines are extrapolations of 2017–19 trends.
Source: Current Population Survey and author’s calculations.
Though other factors may be at play, long COVID has likely contributed to the stalled decline in this series. As evidence, Figure 6 plots the share of individuals who are simultaneously (i) out of the labor force due to disability and (ii) experiencing serious cognitive difficulties. Among women and among non–college graduates—two groups, again, especially affected by long COVID—this share has been trending up over the course of the pandemic. Since not all individuals with long COVID have serious cognitive impairments, the increases in these series are likely a lower bound on the effect of long COVID on disability-driven non-participation.
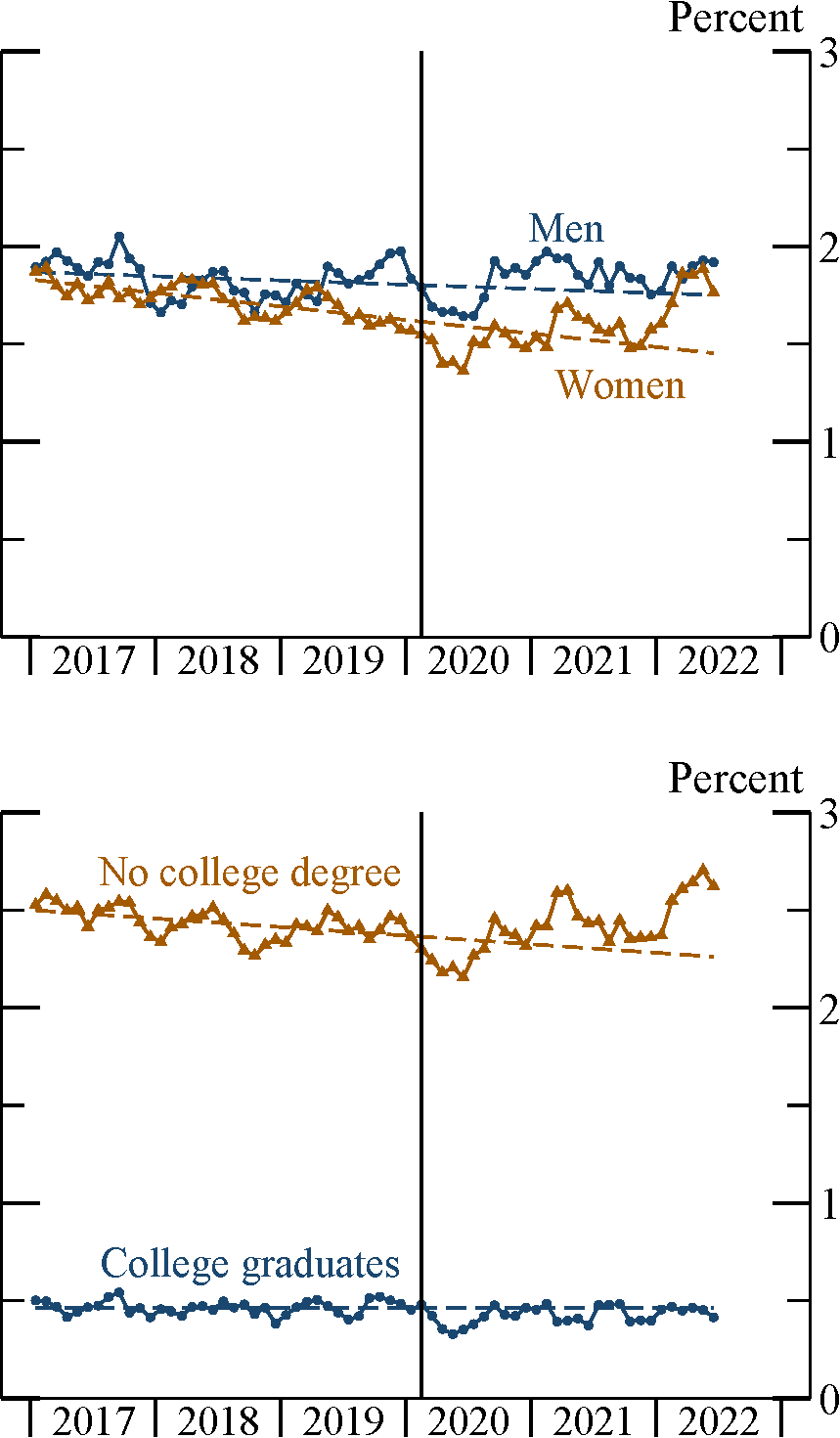
Note: Note: Sample is restricted to ages 18–64. Vertical bar indicates February 2020. Dashed lines are extrapolations of 2017–19 trends.
Source: Current Population Survey and author’s calculations.
III. Conclusion
Long COVID is associated with significant physical, cognitive, and psychological impairments that interfere with activities of daily life. Alongside their effects on health status and quality of life, long-term symptoms of COVID are likely to limit work capacity as well.
My evidence of labor market effects is not conclusive. Regressions in the Household Pulse Survey are consistent with negative effects of long COVID on individual employment rates, but these results are potentially biased by unobserved confounders. Long COVID has likely contributed to the stalling out of the trend decline in disability rates, but its quantitative importance is difficult to assess.
More research is needed. Long COVID appears to be a common condition, especially for some demographic groups, and has the potential to curtail employment, labor force participation, and hours worked. But much is still unknown about its medical causes, its labor market effects, and its future trajectory, which will depend on both the course of the pandemic and the duration of symptoms experienced by long haulers. Recent trends in disability rates also warrant further study, whatever long COVID's role in shaping them.
References
- Bach, Katie (2022), "Is 'Long Covid' Worsening the Labor Shortage?" Brookings Institution, January 11.
- Currie, Janet, and Brigitte C. Madrian (1999), "Health, Health Insurance, and the Labor Market", Handbook of Labor Economics, Vol. 3C: pp. 3309–3416.
- Flood, Sarah, Miriam King, Renae Rodgers, Steven Ruggles, J. Robert Warren, and Michael Westberry (2021), "Integrated Public Use Microdata Series, Current Population Survey: Version 9.0" [dataset]. Minneapolis, MN: IPUMS.
- Goda, Gopi Shah, and Evan J. Soltas (2022), “The Impacts of Covid-19 Illnesses on Workers,” Stanford University and MIT working paper.
- Ham, Dasom (2022), "Long-Haulers and Labor Market Outcomes", Federal Reserve Bank of Minneapolis Opportunity and Inclusive Growth Institute Working Paper No. 60.
- Household Pulse Survey, US Census Bureau.
- Lahart, Justin (2022), "The Economy Could Have a Case of Long COVID", The Wall Street Journal, July 8.
- UC Davis Health (2021), "Studies Show Long-Haul COVID-19 Afflicts 1 in 4 COVID-19 Patients, Regardless of Severity", March 30.
Acknowledgements
The views expressed here are strictly those of the author and do not necessarily represent the views of the Federal Reserve Board or its staff, nor those of the US Census Bureau or the Bureau of Labor Statistics. I am grateful to Andrew Figura, Charles Fleischman, and Ivan Vidangos for helpful comments.
1. See, for example, Bach (2022) and Lahart (2022). Using an event-study design, Goda and Soltas (2022) find that workers who experience week-long health-related absences during the pandemic are 7 percentage points less likely to be in the labor force one year later, compared with otherwise-similar workers who do not experience such absences. Their estimates encompass several possible mechanisms, one of which is long COVID, and imply that COVID-19 illnesses have reduced the US labor force by about 500,000 individuals. Return to text
2. Ham (2022) finds large effects of long COVID on employment as of mid-2021 using data from the Understanding America Study, a survey of about 6000 adults. Return to text
3. The listed symptoms include "tiredness or fatigue, difficulty thinking, concentrating, forgetfulness, or memory problems (sometimes referred to as 'brain fog'), difficulty breathing or shortness of breath, joint or muscle pain, fast-beating or pounding heart (also known as heart palpitations), chest pain, dizziness on standing, menstrual changes, changes to taste/smell, or inability to exercise". Return to text
4. I exclude from the sample individuals with missing values for COVID status, long COVID status, the timing of symptoms, current symptom status, or employment status. When respondents do not indicate whether they have difficulty with a given activity, I assume that they do not. I recode individuals who say they cannot do an activity at all as having "a lot" of difficulty doing so. Return to text
5. See UC Davis Health (2021). Estimates of the frequency of long COVID range widely, in part because the condition has no agreed-upon definition. Studies differ in the set of qualifying symptoms, the population studied, reliance on medical data versus self-reports, and the horizon at which symptoms are measured. Return to text
6. Similar qualitative patterns obtain in a multivariate regression that controls simultaneously for gender, age, race or ethnicity, and educational attainment, along with further controls for survey week, Census region, marital status, and parental status. Differences in long COVID across age groups primarily reflect differences in the likelihood of having had a diagnosed case of COVID, whereas disparities by gender and by educational attainment are mainly driven by differences in the prevalence of long COVID conditional on diagnosed COVID. Hispanics are significantly more likely to have been diagnosed with COVID and somewhat more likely to go on to contract long COVID. Return to text
7. The qualitative patterns shown in Figure 2 continue to hold in regressions that control for a rich set of demographic variables (three-way interactions of gender and educational attainment with survey wave, age bins, race or ethnicity, region, marital status, and parental status). In particular, I find that "at least some" cognitive difficulty is 32 percentage points (pp) more common among long haulers than among those who never had COVID, while "a lot" of difficulty is 13 pp more common. Return to text
8. See, for example, Currie and Madrian (1999). Return to text
9. The trend decline in non-participation due to disability began around 2015. Though its cause is unclear, possible contributors include changing demographics, changes in the structure of the disability insurance program (such as field office closures and changes in appellate rules), and a strengthening labor market providing more work opportunities for disabled individuals in the late 2010s. Data from the Social Security Administration show that applications for Social Security Disability Insurance benefits, which were similarly declining in the lead up to the pandemic, no longer appear to be doing so. Return to text
Price, Brendan M. (2022). "Long COVID, Cognitive Impairment, and the Stalled Decline in Disability Rates," FEDS Notes. Washington: Board of Governors of the Federal Reserve System, August 5, 2022, https://doi.org/10.17016/2380-7172.3189.
Disclaimer: FEDS Notes are articles in which Board staff offer their own views and present analysis on a range of topics in economics and finance. These articles are shorter and less technically oriented than FEDS Working Papers and IFDP papers.